Role of Surgi-ORC® Fibril and SURGISPON® in Posterior Fossa Tumor Resections

What is Posterior Fossa Tumor?
Posterior fossa tumors are a type of brain tumor, though relatively rare, can have a significant impact on an individual’s health and well-being. This area is located at the base of the skull, near the brainstem and cerebellum, these tumors can disrupt vital functions like movement and breathing. While the exact cause remains unknown, they often originate from the meninges, the protective layers surrounding the brain and spinal cord. Tumors of the posterior fossa can be seen in both adults and children with 65% of pediatric brain tumors arising in the posterior fossa [1].
 Fig.1: Anatomy of Brain showing posterior fossa area
Fig.1: Anatomy of Brain showing posterior fossa area
[Image source:https://www.ncbi.nlm.nih.gov/books/NBK65981/]
Symptoms:
The symptoms associated with posterior fossa tumors can vary based on their size and location. However, several common signs may indicate their presence:
- Double Vision: Sudden onset of seeing two of the same object.
- Changed Hearing: Hearing loss or changes in how sounds are perceived.
- Facial Pain or Numbness: Pain or numbness in the face due to nerve compression.
- Headaches: Persistent and severe headaches caused by increased pressure inside the skull.
- Walking Problems: Difficulty walking or maintaining balance due to cerebellar involvement.
- Nausea: Feelings of sickness or vomiting, often related to the brain’s regulation of bodily functions.
- Vertigo: Sensations of dizziness or spinning.
- Problems with Balance: Difficulty in maintaining posture or standing upright.
Types of Posterior Fossa Tumors:
During surgery, tissue samples are taken for lab testing to identify the type of tumor, which usually takes 4-6 weeks. Tumor types in this location include:
- Cerebellar Metastasis: Secondary tumors spreading from other body parts.
- Haemangioblastomas: Slow-growing tumors from blood vessels, often linked to Von Hippel-Lindau Disease.
- Meningiomas: Benign tumors from the brain’s protective tissue.
- Astrocytomas, Medulloblastomas, and Ependymomas: Rare in adults, more common in younger individuals.
- Epidermoid cysts: Benign growths of skin cells in the brain cavity, potentially causing symptoms if compressing vital brain structures [2].
Treatment Options:
Early detection and intervention are crucial in managing posterior fossa tumors. Resection is the primary treatment measure for patients with posterior fossa tumors (PFTs) however, other treatment options may include surgery, radiation therapy, or chemotherapy, depending on the tumor’s size, location, and characteristics [3].
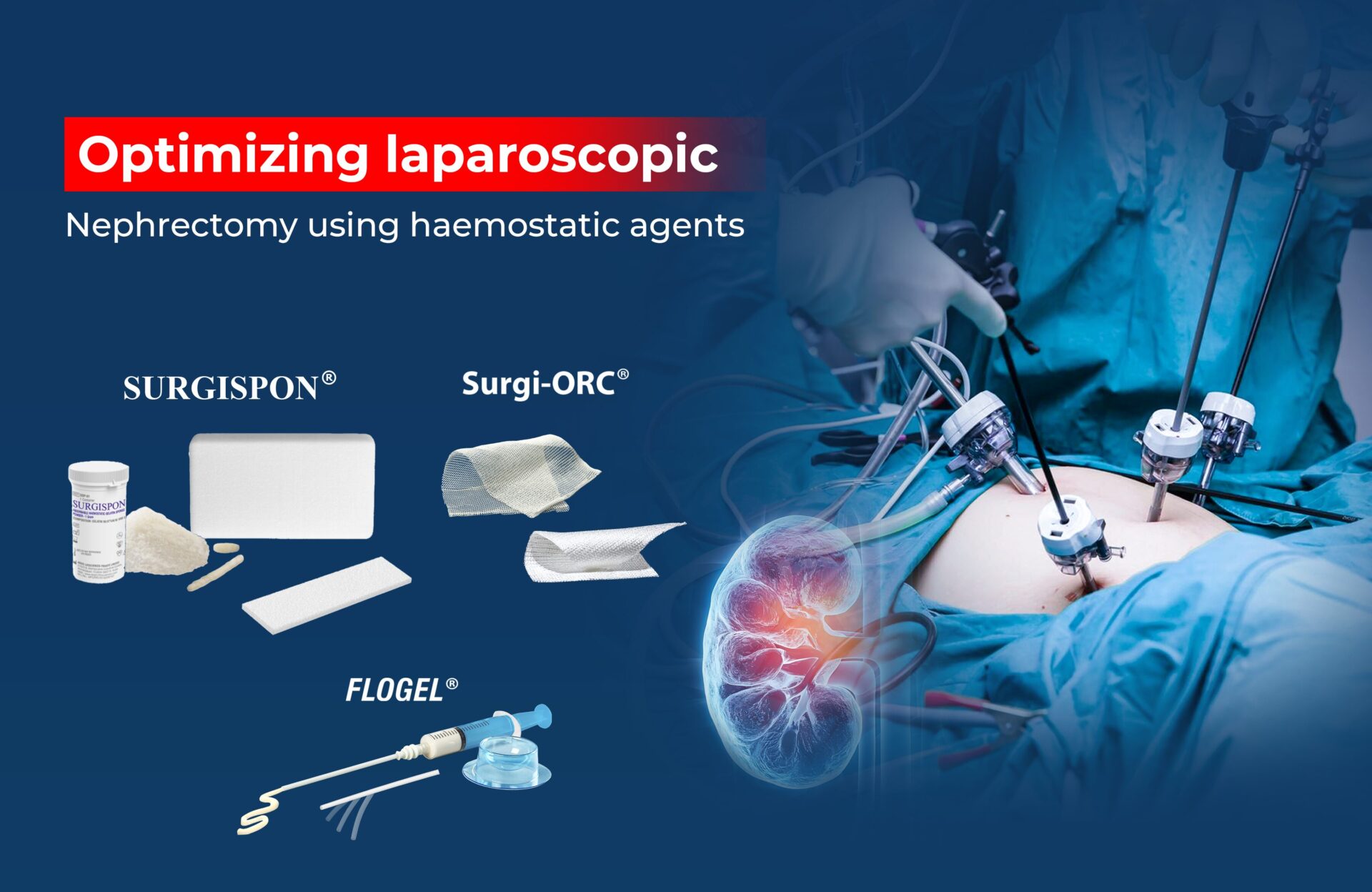
Surgi-ORC® Fibril and SURGISPON®:
At Aegis Lifesciences, we offer advanced hemostatic solutions for posterior fossa tumor reoperations. Surgi-ORC® Fibril, a lightweight and flexible absorbable hemostat made from oxidized regenerated cellulose, provides optimal hemostasis while conforming to irregular surgical sites. SURGISPON®, an absorbable gelatin sponge, offers rapid and effective hemostasis, reducing intraoperative bleeding and surgery time.
Surgeon’s Feedback:
Surgeons at AO Medical in Colombia have successfully used Surgi-ORC® Fibril and SURGISPON® during posterior fossa tumor reoperations. They appreciate the performance and efficiency of these hemostatic agents, minimizing material waste and ensuring effective hemostasis. The pictures of the surgery are shown below:

Fig.2: A) Application of Surgi-ORC® fibril along with SURGISPON® at the posterior fossa tumor reoperation
(B) & (C) Absorption of both haemostats
[Image Source: AO Medical, Colombia].
References:
[1] Bray HN, Sappington JM. A Review of Posterior Fossa Lesions. Missouri Medicine. 2022 Nov;119(6):553.
[3] Zhang C, Zhang T, Ge L, Li Z, Chen J. Management of posterior fossa tumors in adults based on the predictors of postoperative hydrocephalus. Frontiers in surgery. 2022 Jun 1;9:886438.