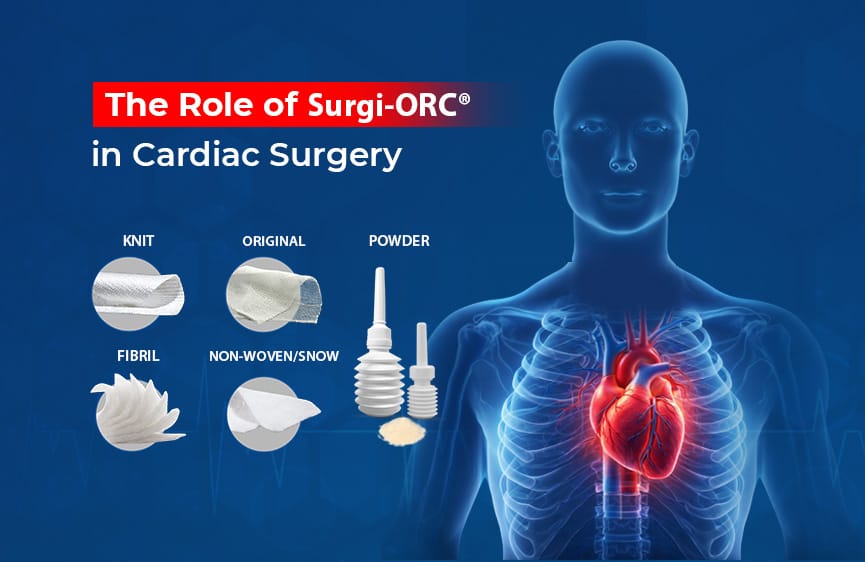
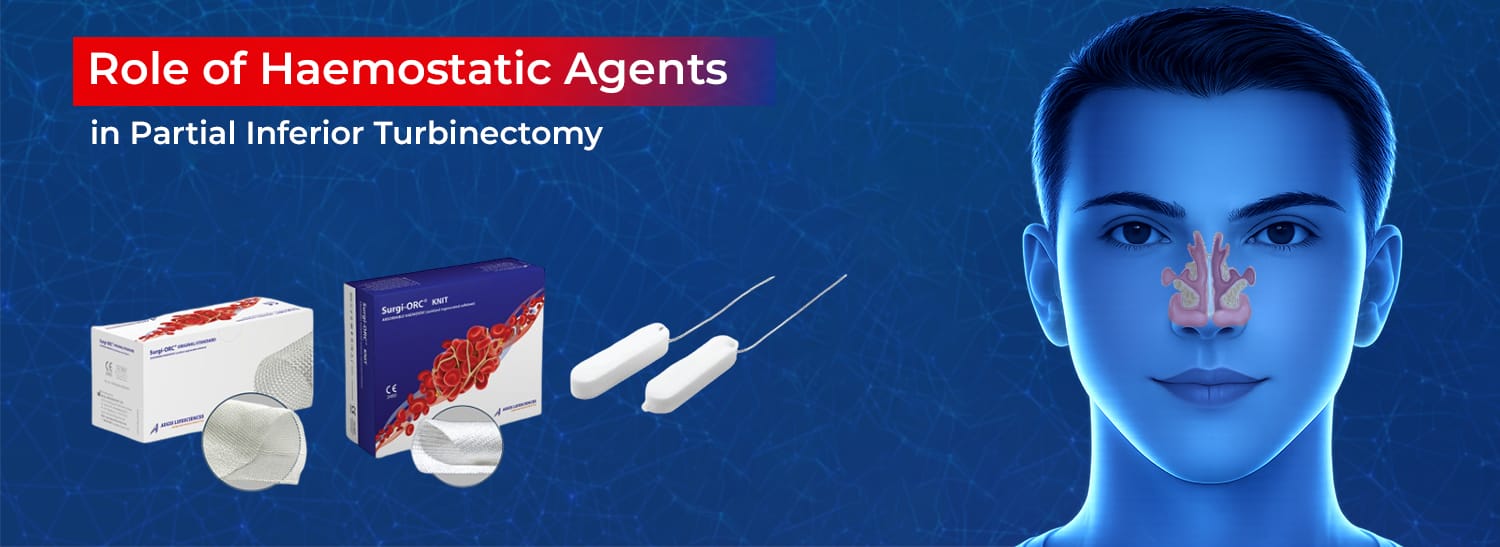
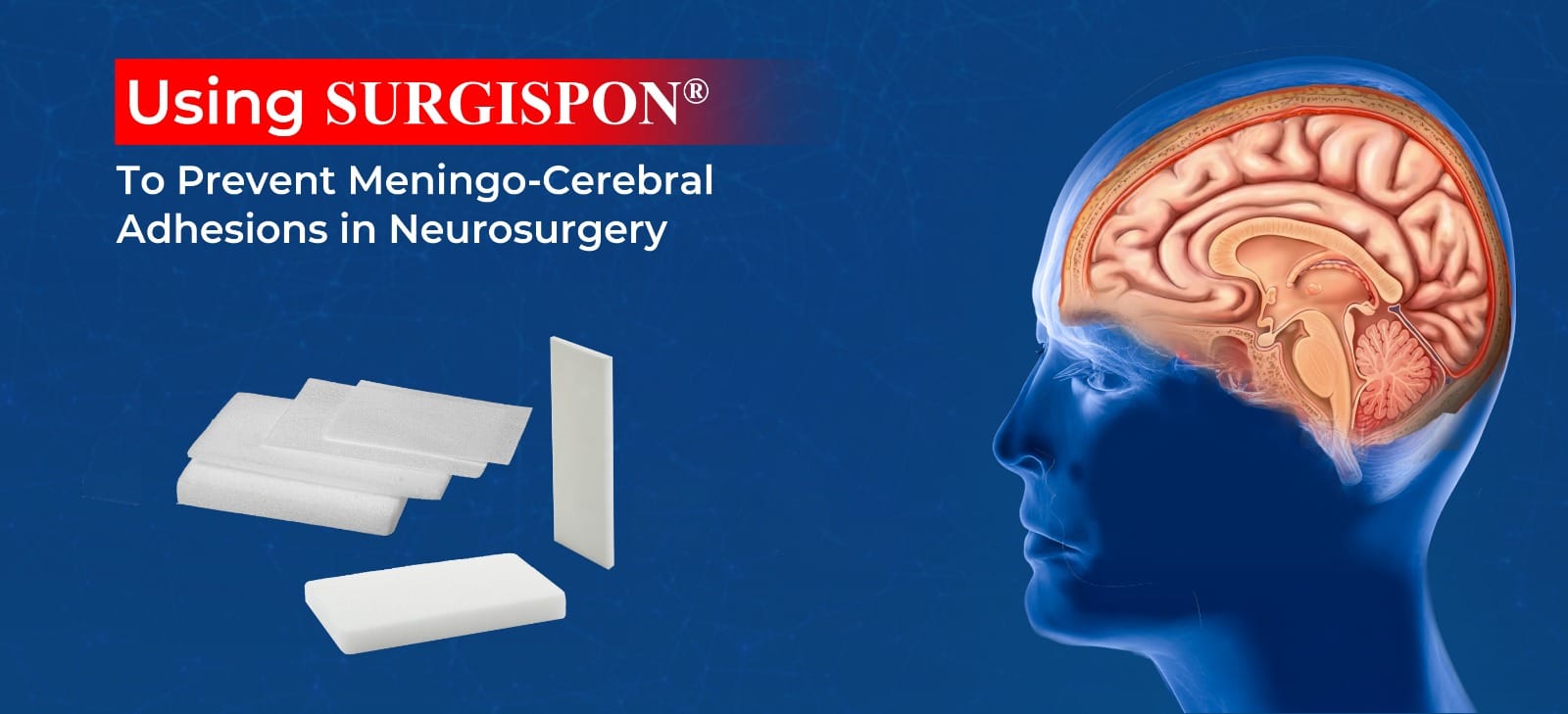
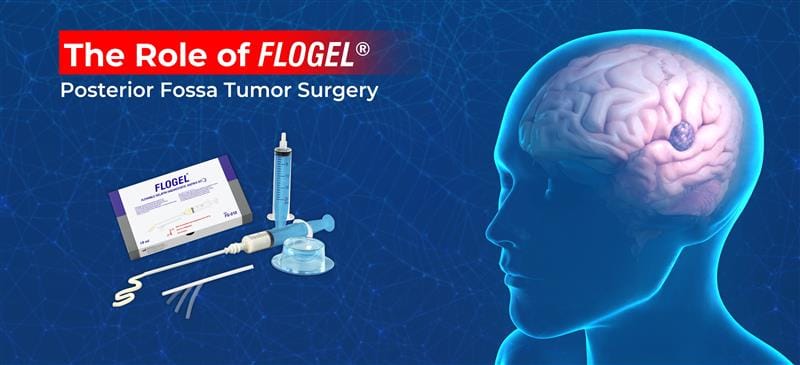
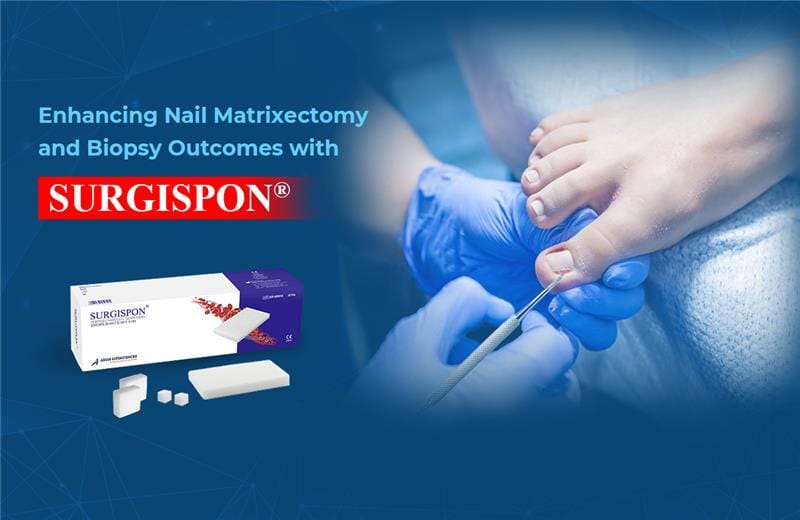
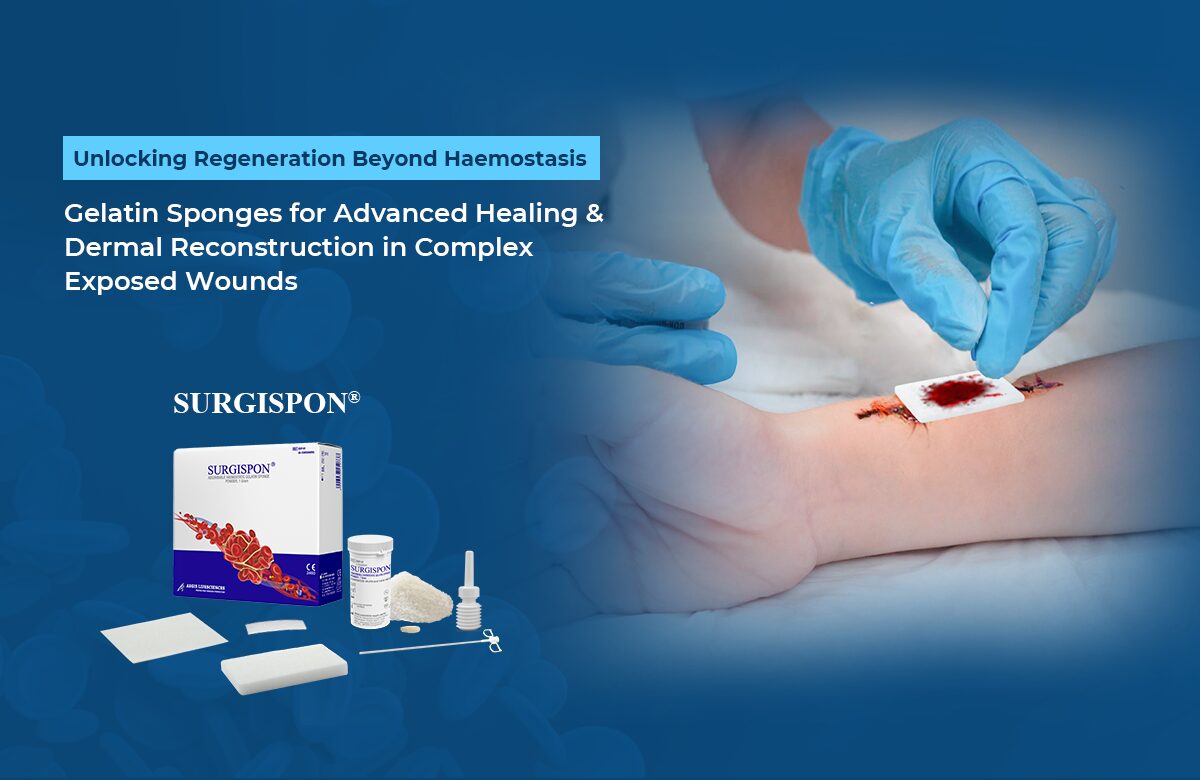
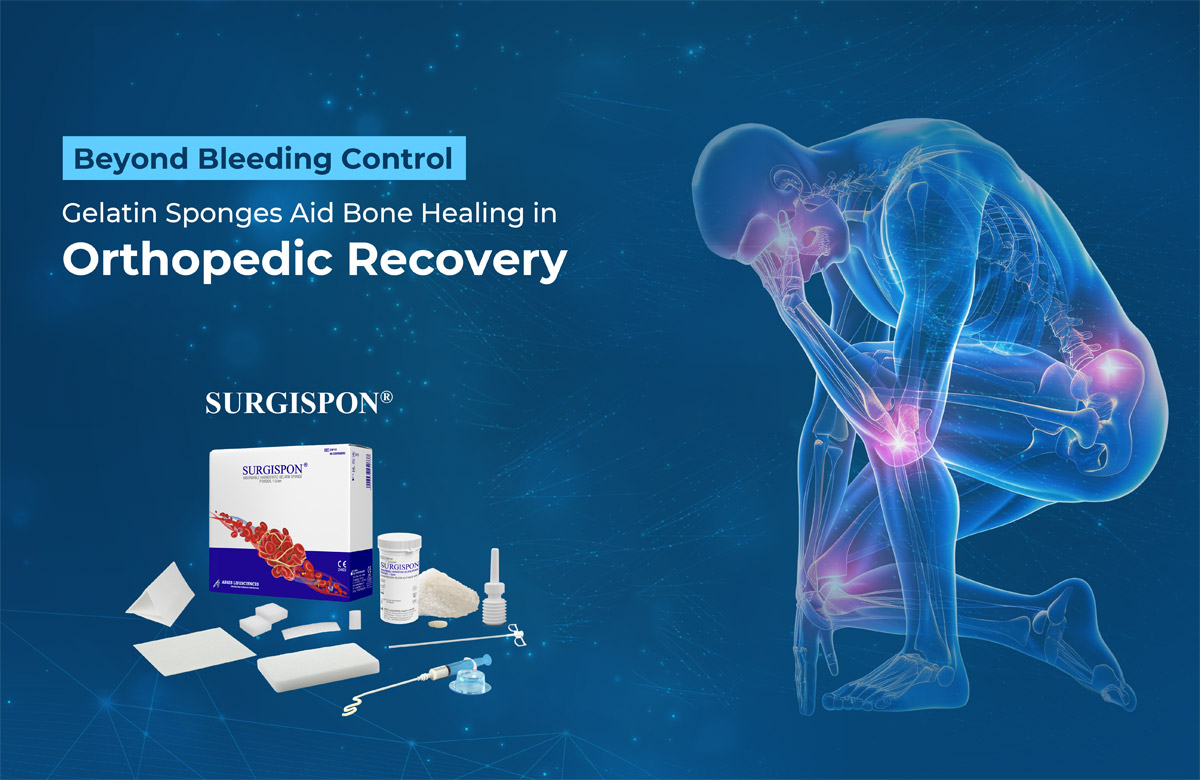
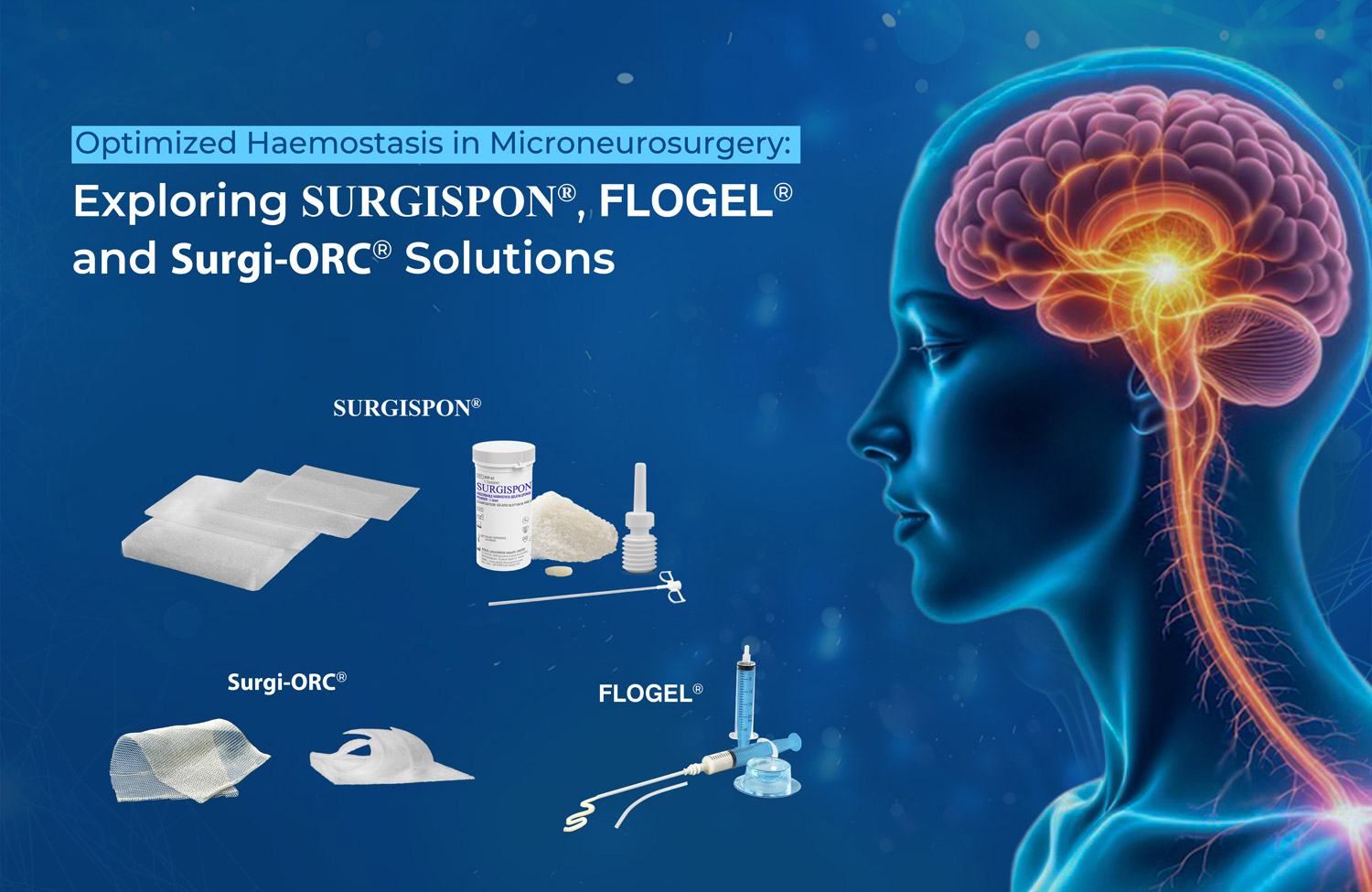
Role of SURGISPON®/ HAEMOVET® in Dog’s Dental Surgery

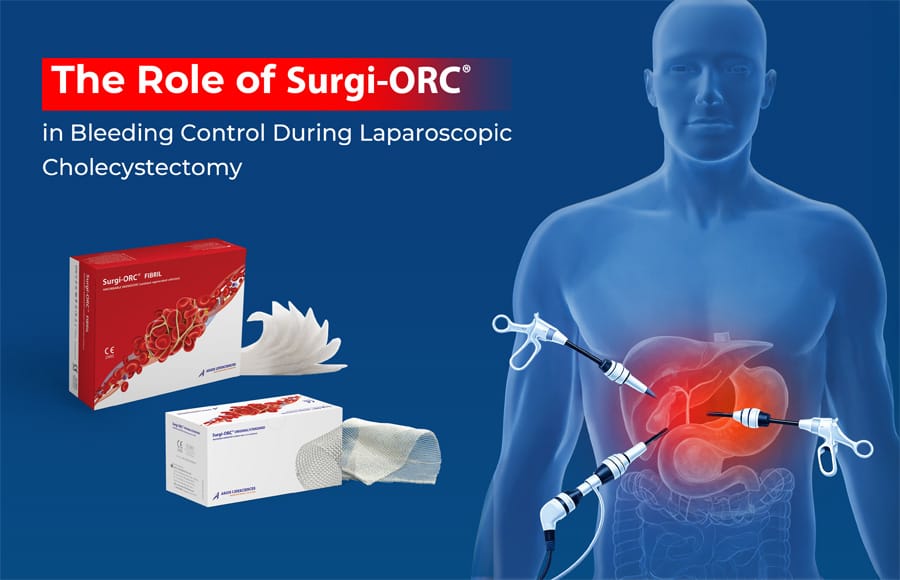
Clefts of the lip, alveolus, and palate are among the most common craniofacial birth abnormalities found in both humans and animals. Traditional treatments, such as autogenous bone grafts, have long been regarded as the gold standard. However, these methods have substantial disadvantages, including limited bone availability and donor-site problems such as post-operative pain, changes in sensation, and the risk of infections and scarring. Fortunately, recent approaches in cell therapy and tissue engineering provide promising solutions to these issues. One interesting strategy is to use a gelatin sponge scaffold combined with cultured stem cells to repair cleft alveoli in dogs. In this blog, we’ll explore how combining these innovative approaches particularly utilizing a gelatin sponge scaffold with cultured stem cells, can revolutionize the treatment of craniofacial defects in dogs.
Role of Gelatin Sponge, Cell therapy, and Tissue Engineering
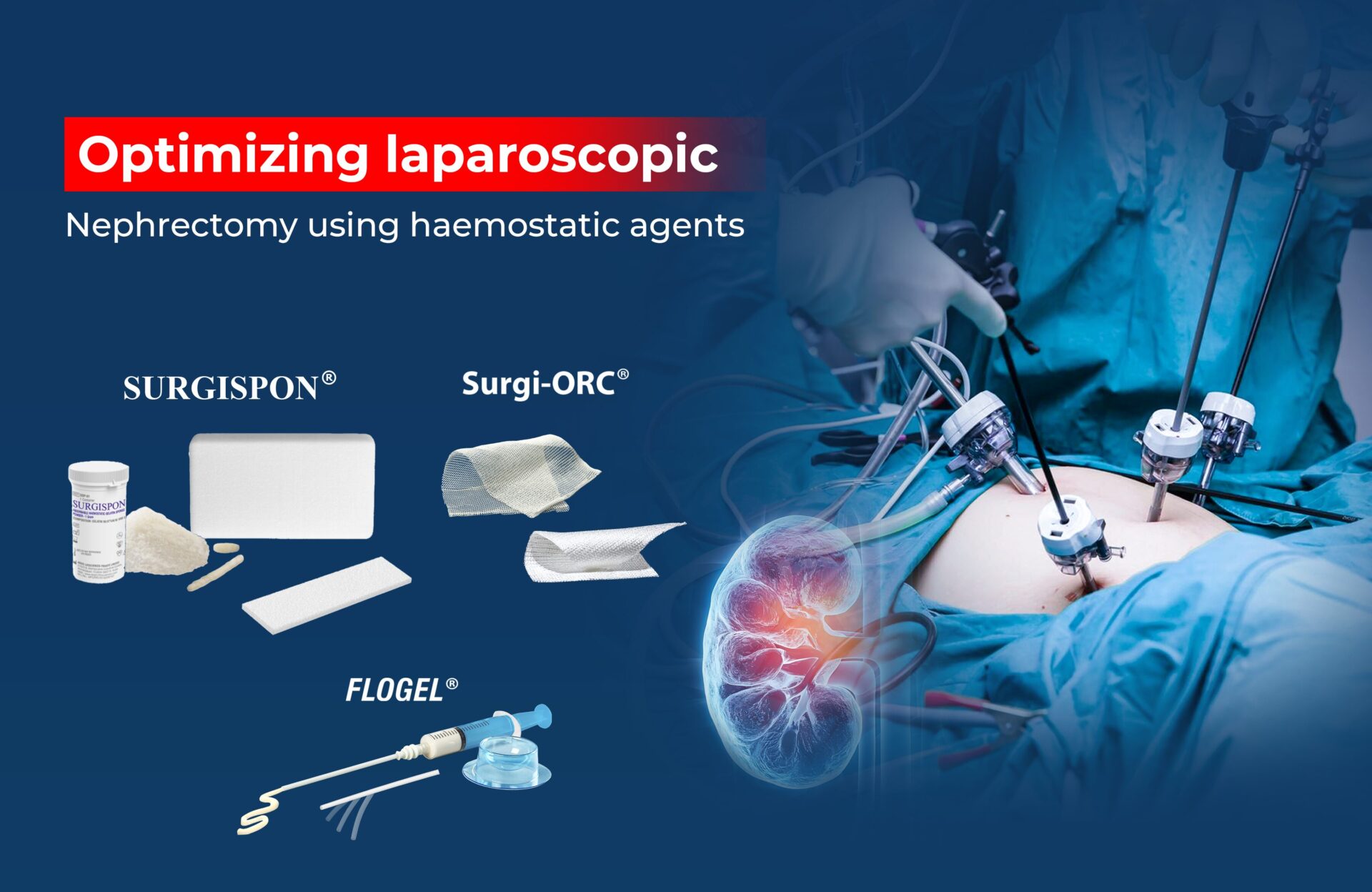
Gelatin Sponge Scaffold: The gelatin sponge acts as a three-dimensional scaffold, providing structural support to the repair site. Its porous shape enables for the penetration of cells and growth substances, which promotes tissue regeneration and repair.
Cell therapy: It involves the use of stem cells, which have the unique capacity to differentiate into multiple cell types such as bone and soft tissue cells. These cells can be obtained from the patient’s own tissues or from compatible donors which lowers the chance of rejection and other complications.
Tissue engineering enhances cell treatment by creating a favourable environment for cell proliferation and tissue regeneration. Gelatin sponge excels in hemostasis, which ensures that blood flow is efficiently controlled. This is especially important in veterinary surgery, when patients are unable to verbalise their distress, making precision and safety critical. In some circumstances, gelatin sponge serves as a scaffold for bone graft materials, facilitating the formation of new bone and tissue regeneration.Gelatin is notable for being both absorbent and non-adherent. It will eventually absorb within the body after it serves its purpose of controlling bleeding. This eliminates the need for a second surgery to remove it resulting indecreasing post-operative complications and ensuring a faster and smoother recovery for the animal patient.
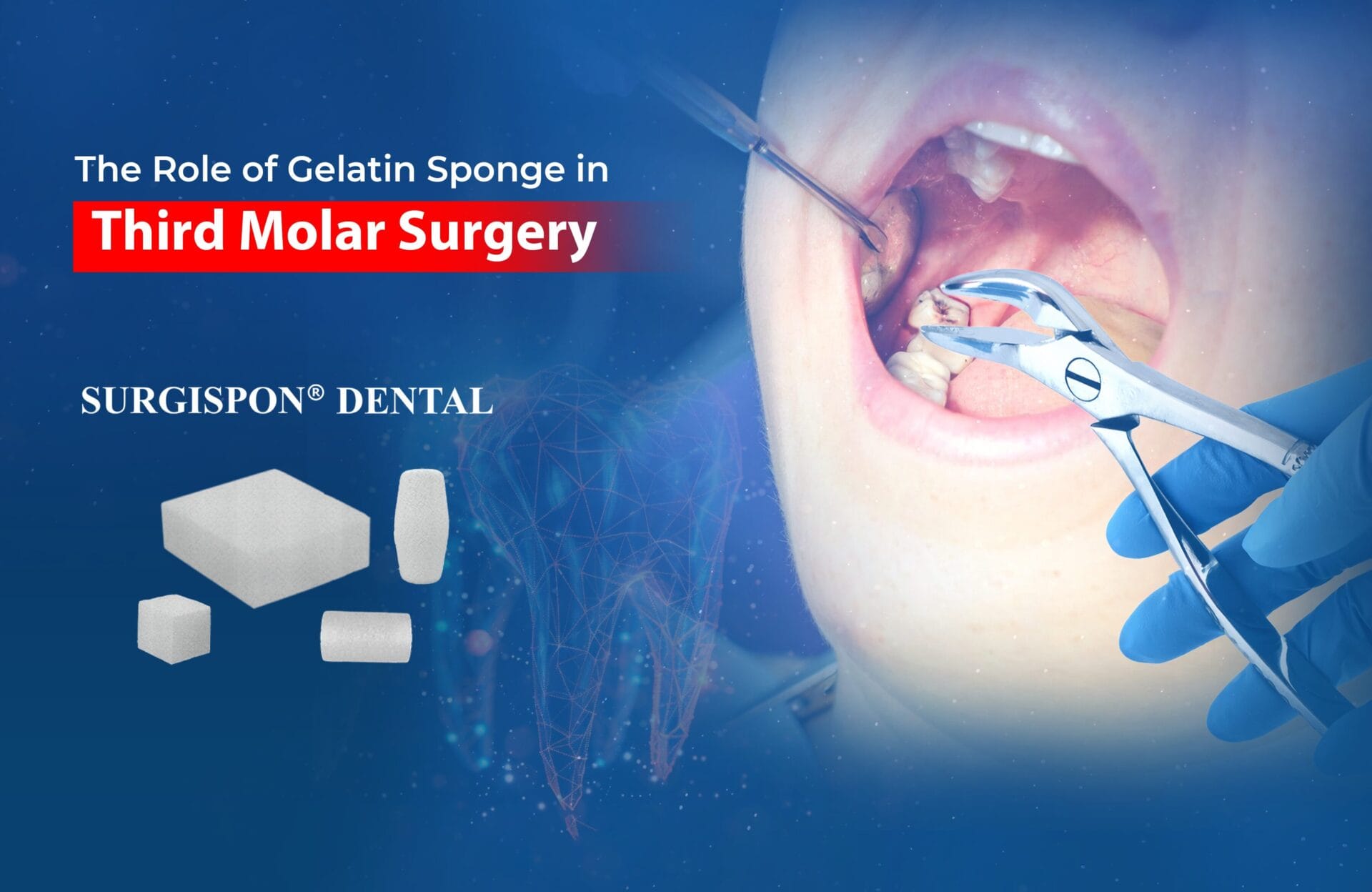
Clinical Veterinary Study Insights:
A Clinical Veterinary Study involving 12 healthy mongrel dogs utilized Gelatin Sponge (SURGISPON®, Aegis Life Science, India) as a scaffold, along with stem cells, to repair alveolar bone defects.This study concluded that stem cells cultured on gelatin scaffold accelerated the healing and regeneration of alveolar cleft and new bone formation in dogs [1].

Fig.1: A. The surgical site was covered with sterile surgical towels. B. A standardized alveolar bone defect defects (0.8Å~0.5Å~0.5 mm). C. The defect filled with a scaffold Surgispon® (Aegis Life Sciences) [1].
Further Advancements:
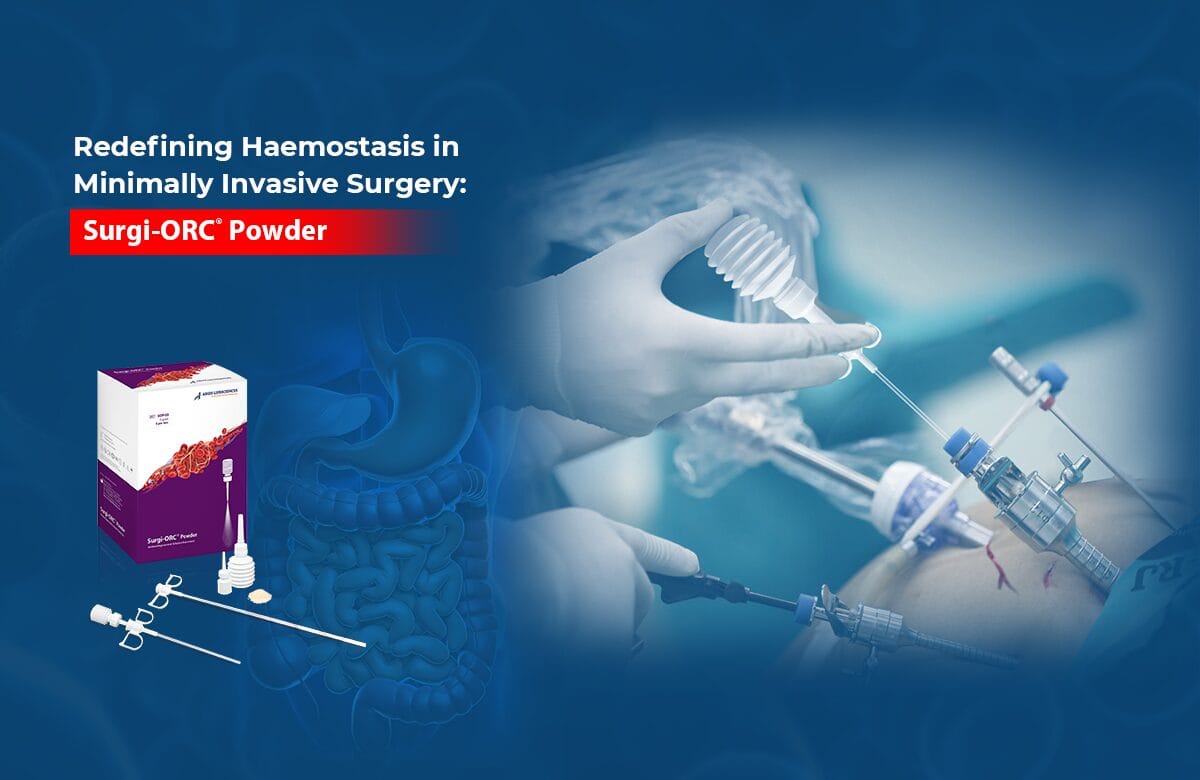
Aegis Lifesciences has introduced a new product HAEMOVET® Dental sponges which comprised of Absorbable Gelatin Sponge and offer alternatives for veterinary dental surgeries. When implanted in tissues in appropriate amounts, it completely absorbs within <4 weeks. In oral and dental surgery, HAEMOVET® Sponges serve as a valuable aid in achieving hemostasis. HAEMOVET® may be used either dry or moistened, depending upon conditions present at operation and preference of the surgeon. Isotonic saline is suitable for use with HAEMOVET®.
Additionally, HAEMOVET® Dental sponge, impregnated with colloidal silver, provides additional antibacterial properties, ensuring optimal healing conditions in the oral cavity.

HAEMOVET® Dental Sponge

HAEMOVET® Silver Sponge
References
- Eman A. El Ashiry, Najlaa M. Alamoudi, Reem M. Allarakia, Amr M. Bayoumi, Essam E. Ayad, Amani A. Al Tuwirqi, Maha M. Mounir, RahafSahhaf, Mohmed A. Abd El hamid, Omar A. El Meligy. Histological and histomorphometrical evaluation of adipose tissue and bone marrow-derived mesenchymal stem cells in regeneration of the cleft alveolus in dogs. Medical Science, 2020, 24(102), 750-764.
http://www.discoveryjournals.org/medicalscience/current_issue/v24/n102/A41.pdf